Healthcare Revenue Cycle Management
Medical Practice Revenue Cycle Management: Fix Cash Flow Leaks
Medical practice revenue cycle management helps reduce denials, improve cash flow, and streamline billing from patient scheduling to final payment.
TL;DR — Quick Takeaways
- Medical practice revenue cycle management covers every financial step from appointment booking to final reimbursement.
- Most revenue leaks begin with preventable front-end issues like registration errors, missed authorizations, and weak eligibility checks.
- Clean coding, claim scrubbing, denial management, and accurate payment posting are essential to faster cash flow and lower write-offs.
- A specialized nearshore BPO partner like CallZent can improve collections, reduce administrative burden, and free staff to focus on patient care.
Is your medical practice’s cash flow more of a rollercoaster than a steady stream? If so, you’re not alone. Many practices unknowingly lose a significant portion of their revenue to small, preventable mistakes buried in their financial processes.
This is where expert Medical Practice Revenue Cycle Management (RCM) becomes a game-changer. It’s not just an industry buzzword; it’s the end-to-end administrative and financial journey that tracks a patient from the moment they book an appointment until their balance is paid in full. Simply put, it’s the financial lifeblood of your practice.
What is Medical Practice Revenue Cycle Management?
Think of your practice’s revenue cycle like its circulatory system. When it flows smoothly, cash moves predictably, keeping the business healthy and strong. But even one tiny blockage—a simple data entry error at check-in or a single missed pre-authorization—can obstruct the flow, leading to denied claims, delayed payments, and lost income.
This is why so many practices get stuck in a “feast-or-famine” cycle. While some resources talk about ending feast-or-famine revenue cycles in other fields, the core challenge is identical: creating stable, predictable cash flow. Mastering your medical RCM is how you achieve that stability.
This flow chart gives you a bird’s-eye view of how the process is supposed to work, moving from the patient’s appointment to the insurer’s payment.
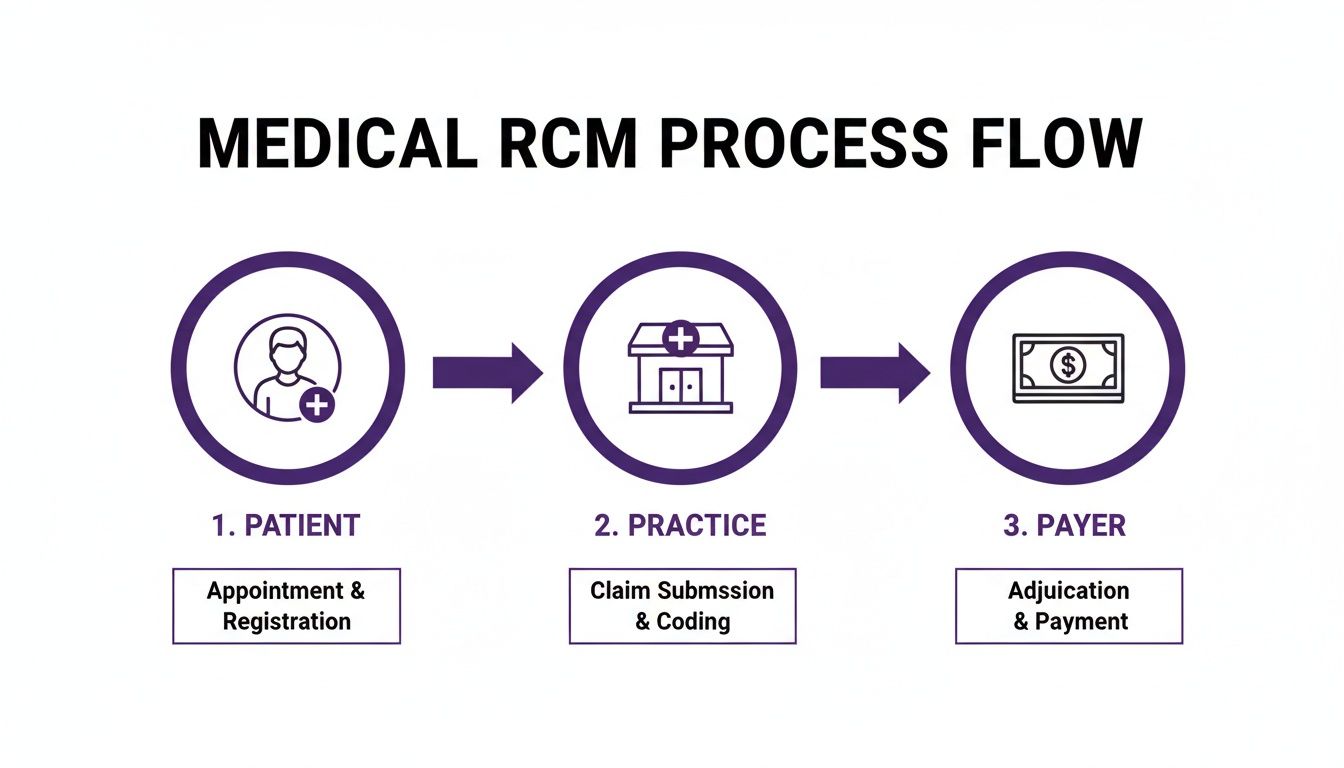
As you can see, it’s a three-way street between the patient, the practice, and the payer. A successful outcome depends entirely on seamless handoffs between all three.
The Real Cost of Inefficient RCM
Broken RCM processes don’t just delay payments; they actively drain your practice’s profitability. The pain points are all too common:
- Rising Claim Denials: Incorrect patient data or coding mistakes create a mountain of rejected claims that your staff has to rework, eating up valuable time.
- High Days in Accounts Receivable (AR): When it takes too long to get paid, your cash flow tanks, making it harder to cover payroll, rent, and other operational costs.
- Administrative Overload: Your team gets stuck chasing payments and fixing billing errors instead of focusing on what they do best—delivering great patient care.
Optimizing your revenue cycle isn’t just about getting paid; it’s about building a financially resilient practice that can thrive and grow.
Here’s a practical example. A busy clinic that doesn’t consistently verify insurance eligibility before appointments could easily see a 15% denial rate. That one small slip-up on the front end forces the back-office team into a reactive loop of appeals and collections, hitting the bottom line hard. It also sours the patient experience when they get hit with an unexpected bill.
This is where a strategic partner like CallZent can make all the difference. Specialized BPO firms live and breathe this stuff. They bring expert teams and technology to manage every step, from scheduling and pre-authorizations to denial management. By taking over these complex administrative tasks, they free up your team to focus on patients. This is especially true when it comes to patient communication, where professional support can turn a potential headache into a positive interaction. You can learn more in our guide on after-hours medical answering services.
Mastering the Front-End RCM Process
Your biggest financial leaks probably aren’t in the back office. They start right at your front desk. This “front-end” of the medical practice revenue cycle is the foundation for your practice’s entire financial health, and it’s where a little prevention saves a ton of headaches later.
Think of it like building a house. A cracked foundation guarantees problems down the road, no matter how well the rest is built. The same goes for patient pre-registration, scheduling, and insurance verification. Getting these steps right isn’t just a good idea—it’s non-negotiable for a healthy revenue stream.

The High Cost of Small Front-End Errors
A tiny, seemingly harmless mistake during check-in can spiral into a major financial headache weeks or even months later. It’s a classic domino effect that silently drains your practice’s time and money.
Here’s a real-world example: a new patient arrives, and a rushed front desk staffer misspells their name by one letter. The insurance ID is correct, but the name mismatch is enough for the payer’s system to automatically kick back the claim.
Weeks later, your billing team gets the denial. Now they have to drop what they’re doing to:
- Dig into the reason for the denial.
- Hunt down the original patient chart.
- Spot the typo and correct it.
- Resubmit the entire claim and restart the payment clock.
All that rework—the wasted hours and delayed cash flow—was completely avoidable. In fact, studies show that up to 80% of claim denials are preventable, with a huge chunk stemming from simple front-end slip-ups like demographic errors or eligibility issues.
Perfecting Patient Registration and Eligibility Verification
The first two steps—patient registration and insurance verification—are your golden opportunities to stop problems before they start. The goal here is simple: collect and confirm every detail before the patient ever sees a provider.
Your front desk isn’t just a reception area; it’s your first line of financial defense. Empowering them with the right tools and processes is one of the smartest investments a practice can make.
Key actions to lock down this phase of your medical practice revenue cycle management include:
- Pre-registration: Get patient demographic and insurance info before the appointment. This gives your staff breathing room to verify everything without the pressure of a full waiting room.
- Real-Time Eligibility Checks: Don’t just copy the insurance card. Run a real-time check to confirm the policy is active and see what services are covered before the visit. This is crucial for accurately estimating the patient’s out-of-pocket costs.
- Prior Authorization: Pinpoint any services that need a green light from the insurer and get that authorization secured well ahead of time.
Translating Care into Cash with Charge Capture
Once the clinical work is done, the next critical step is charge capture. This is where you translate everything that happened during the visit—every procedure, test, and consultation—into billable codes.
Missed charges are a common pitfall. Forgetting to bill for a routine injection or a quick in-office test is like leaving cash on the table. The same goes for incorrect coding. Both lead directly to lost revenue.
Effective charge capture demands a seamless connection between your clinical notes and your billing system. Integrating a solid system is non-negotiable, and you can learn more about the technology that powers this in our overview of medical practice management software.
Ultimately, mastering the RCM front-end is about moving from a reactive to a proactive mindset. When you invest in getting clean, accurate, and verified data from the get-go, you stop fires before they start. The result is a smoother, faster, and more profitable revenue cycle.
Navigating Medical Coding and Claim Submission
The work doesn’t stop when the patient walks out the door. In fact, that’s when the critical middle part of your revenue cycle kicks in—the part where clinical care gets translated into a financial claim. If the front-end work is your foundation, think of this stage as the crucial framing and wiring of your practice. Mistakes here will cause major system failures down the line.
At the heart of this process are medical codes. These aren’t just arbitrary numbers; they are the universal language spoken between your practice and the insurance payers. Every claim tells a story using two main types of codes:
- ICD-10 Codes: These are diagnostic codes. They answer the question, “Why was the patient seen?” by describing their illness, injury, or symptoms.
- CPT Codes: These are procedural codes. They answer, “What was done for the patient?” by detailing every single service, test, and treatment you provided.
Getting this language exactly right is non-negotiable. One wrong code can create confusion, trigger payment delays, or lead to a flat-out denial.
Clean Claims vs. Dirty Claims in Your Revenue Cycle
After coding, the claim starts its journey to the payer. Ideally, it’s a clean claim—one that is perfectly accurate, complete, and formatted correctly from the get-go. These claims sail right through the system, often getting processed and paid automatically in just a few weeks.
A dirty claim, on the other hand, is any claim that has an error. This could be anything from a simple coding mismatch to missing patient information. These are the claims that get stuck, flagged for a manual review, or denied, forcing your staff to burn valuable time figuring out what went wrong and how to fix it. This rework is a direct drain on your practice’s resources and profitability.
Every dirty claim represents a breakdown in the process and a delay in receiving the revenue you’ve already earned. The goal is to maximize your clean claim rate on the first submission.
The Power of Claim Scrubbing in Medical Practice RCM
So, how do you stop dirty claims before they ever leave your office? The answer is a process called claim scrubbing.
This is your quality control checkpoint. Before a claim is shot off to the payer, it’s run through a “scrubber”—which can be specialized software or an expert team that audits it for all the common errors.
This scrubbing process double-checks for things like:
- Valid and compatible ICD-10 and CPT codes.
- Correct patient demographic and insurance information.
- Proper use of modifiers.
- Compliance with specific payer rules and regulations.
Think of it like a spell-checker for your medical claims. It catches potential mistakes before they can cause a denial, dramatically boosting the chance of getting paid correctly on the first try. A good scrubbing process can push a practice’s first-pass acceptance rate above 95%, which has a massive, positive impact on cash flow.
For many practices, managing this complex coding and submission process in-house is a huge challenge. This is where a dedicated partner can provide immense value. You can find out more about how specialized teams handle these tasks in our guide to healthcare BPO services. By entrusting this critical middle stage to experts, you ensure every claim is accurate, compliant, and optimized for fast payment.
Solving Denials and Optimizing the Back-End RCM
There’s nothing quite as deflating for a medical practice as a denied claim. You’ve delivered top-notch care, wrestled with the paperwork, and after weeks of waiting, a rejection lands on your desk instead of a payment. This back-end of the revenue cycle—denial management and payment posting—is where financial battles are truly won or lost.
But here’s the thing: this isn’t just a reactive cleanup chore. It’s a strategic intelligence mission. Every single denial is a data point, a breadcrumb leading you straight to a crack in your process. If you can turn that frustration into a fact-finding mission, you won’t just recover lost revenue—you’ll stop it from leaking out in the first place.

Turning Denials Into Strategic Intelligence
Claim denials aren’t random. They happen for specific, traceable reasons, and getting to the bottom of them is the only way to fix your revenue stream for good.
While reasons can vary, most rejections fall into a few familiar buckets.
Common Culprits Behind Claim Denials:
- Missing or Incorrect Patient Information: Simple typos in a name, a wrong date of birth, or an outdated policy number are the low-hanging fruit for automated rejections.
- Lack of Prior Authorization: Many procedures need a green light from the insurer beforehand. Skipping this step is a guaranteed denial.
- Coding Errors: The wrong CPT or ICD-10 code, or a mismatch between the diagnosis and the service provided, will get a claim flagged almost instantly.
- Filing Past the Deadline: Payers are sticklers for timely filing limits. Miss that window, and you might as well write off the payment.
Instead of playing whack-a-mole with each denial, the real power move is to analyze the patterns. Is one specific insurer constantly rejecting claims for the same reason? Is a particular procedure always missing its authorization? That’s where your denial data becomes a roadmap for fixing the root cause.
A Framework for Effective Denial Management in Your Revenue Cycle
When a denial hits, a systematic approach is your best friend. The goal isn’t just to appeal; it’s to do it quickly, efficiently, and with a high success rate.
- Identify and Categorize: Immediately figure out why the claim was denied and group it with similar rejections.
- Prioritize by Value and Age: Go after the high-dollar claims and those closest to their appeal deadline first.
- Correct and Resubmit: Round up the right documents, fix the error, and get the corrected claim back to the payer through the proper channels.
- Track and Analyze: Log every denial, its cause, and the appeal outcome. This data is pure gold for improving your medical practice revenue cycle management.
On average, medical practices see claim denial rates hovering between 10-15%. A practice that isn’t tracking this can watch their days in accounts receivable (AR) balloon far beyond the healthy 30-40 day benchmark. Today, AI-driven tools are helping providers slash their denial rates by up to 50% and push their first-pass resolution over 90%.
Optimizing Payment Posting for Financial Clarity
Once a claim is finally approved and paid, the job isn’t done. The final piece of the puzzle is payment posting. This might sound like basic data entry, but it’s a critical financial reconciliation step. It’s where you record the payment from the insurer and patient, apply any contractual adjustments, and formally close out the account.
Accurate payment posting is how you confirm you were paid correctly based on your contracted rates. It’s also your first line of defense against underpayments—a surprisingly common issue where payers remit less than they owe. Without meticulous posting, these little shortfalls can fly under the radar, bleeding significant revenue over time. For modern practices, knowing how to integrate a payment gateway is key to making this process smoother and improving cash flow.
A 5% reduction in your claim denial rate can increase your practice’s annual revenue by tens of thousands of dollars.
This is exactly where a dedicated partner shines. Managing denials and posting payments demand a relentless, detail-obsessed team. For many practices, it’s simply too much to handle in-house. Outsourcing this work gives you a specialist team that not only chases every dollar but also provides the analysis you need to strengthen your entire RCM from the inside out. To learn how a dedicated team can handle these complex tasks, check out our guide on back office support with a nearshore BPO.
In-House RCM vs. Outsourcing: When to Make the Switch
Deciding whether to keep your medical practice revenue cycle management in-house or hand it off to a partner is a major strategic choice. It’s not just about cost—it’s about efficiency, expertise, and whether your team can truly focus on patient care.
While running your own RCM team gives you direct control, there are clear trigger points that signal it’s time to seriously consider outsourcing. Spotting these signs early can save your practice from serious financial strain and administrative burnout.
Key Signs It Is Time for an Outsourced RCM Partner
If any of the following sound familiar, it’s a strong indicator that your current RCM process is falling behind and an outsourced partner could turn things around.
- Your Claim Denial Rate Is Creeping Up: This is the most obvious red flag. If your denial rate climbs above the 5-7% industry benchmark, it means your front-end or coding processes are breaking down somewhere. A dedicated RCM partner’s job isn’t just to appeal claims; it’s to diagnose and fix the root cause for good.
- Your Days in A/R Are Too High: Are you waiting 45, 60, or even 90 days to get paid? That kind of delay cripples cash flow. A healthy practice keeps its Days in Accounts Receivable (A/R) below 40. Anything higher points to systemic issues in your claim submission and follow-up that a specialized team is built to resolve.
- High Staff Turnover and Burnout: RCM is a highly specialized and often grueling field. If you’re constantly hiring and training new billing staff, the associated costs and inconsistencies are likely costing you more than you think. Outsourcing gives you a stable, trained team without the HR headaches.
- You Can’t Keep Up with Regulations: Payer rules, coding updates, and compliance requirements change constantly. Staying current is a full-time job. An expert partner invests heavily in continuous training and technology to guarantee compliance, protecting your practice from costly penalties.
Selecting the Right BPO Partner for Your Medical Practice
Once you’ve decided to explore outsourcing, picking the right partner is everything. Not all BPO providers are created equal, especially in healthcare. You need a team that genuinely understands the unique complexities of medical practice revenue cycle management.
Look for a partner that can prove its expertise in these key areas:
- Healthcare-Specific Experience: Do they have a proven track record with practices like yours? They need to speak your language, from CPT codes to HIPAA compliance.
- HIPAA Compliance and Security: This is completely non-negotiable. Your partner must have rock-solid security protocols to protect sensitive patient health information (PHI).
- Transparent Reporting and KPIs: A good partner acts like an extension of your own team. They should provide clear, regular reports on key performance indicators (KPIs) like denial rates, A/R days, and collection rates, so you always know exactly how your financial health is trending.
Your RCM partner shouldn’t be a black box. They should provide total visibility into their performance and your practice’s financial metrics.
The Nearshore Advantage for Medical RCM
When you’re evaluating partners, geography matters. A nearshore partner, like one based in Tijuana, Mexico, offers a unique combination of benefits that are tough to match.
- Time Zone Alignment: Working with a team in a compatible time zone means no more communication lags. Your teams can collaborate in real-time during your business hours, resolving issues in minutes, not days.
- Cultural Affinity: A shared cultural context with the U.S. market leads to much smoother communication with both your staff and your patients, which is especially important during sensitive collection calls.
- Significant Cost Savings: Nearshore partners deliver substantial cost savings compared to a domestic U.S.-based team, but without sacrificing quality or expertise. It’s a powerful way to access top-tier talent at a more sustainable price point.
For a deeper dive into the specific benefits, our guide on outsourcing medical billing companies provides a detailed breakdown. Partnering with a nearshore expert like CallZent gives you the best of both worlds: operational efficiency and strategic financial management.
Your Actionable Checklist for a Better Revenue Cycle
Theory is one thing, but making actual changes to your medical practice’s revenue cycle is where you see results. This final section is all about action. We’ve laid out a simple playbook to help you get started—a mix of quick wins and long-term strategies for building lasting financial health.
Quick Wins for Immediate Impact
Start here to stop the most common revenue bleeds and get fast results. These moves don’t require a huge investment, but they make a real difference by tightening up your day-to-day operations.
- Audit Your Top 5 Denial Reasons: Pull a report of your denials from the last 30 days and find the top five reasons claims are getting kicked back. Is it missing pre-authorizations? Typos in patient data? Make it your team’s mission this week to train on preventing those specific errors.
- Implement a Daily Insurance Verification Protocol: Stop waiting until the patient is standing at the front desk. Make it a rule: every appointment scheduled for tomorrow must have its insurance eligibility verified by the end of today. This single habit knocks out a huge number of front-end denials.
- Review Your Collections Script: How does your team actually sound when they call patients about a balance? Take a hard look at the script. It should be clear, empathetic, and always end with easy ways to pay. A better conversation almost always leads to a faster payment.
Long-Term Strategies for Sustainable Growth
Once you’ve put out the immediate fires, it’s time to build a more resilient and efficient system for the long haul. These strategies take a bit more planning but are what separate struggling practices from thriving ones.
- Develop a KPI Scorecard: You can’t improve what you don’t measure. Create a monthly scorecard tracking your vitals: Clean Claim Rate, Days in A/R, and Denial Rate. Review it with your team to keep everyone accountable and to spot bad trends before they snowball.
- Evaluate Your Practice Management Software: Is your current PM/EHR system working for you or against you? See if it has features like automated eligibility checks, solid claim scrubbing, and reporting that actually gives you insight. If it’s falling short, it might be time to see what better tech is out there.
- Conduct a Fee Schedule Analysis: When was the last time you actually looked at your fee schedule? Compare it against your payer contracts and what other practices in your area are charging. You could easily be undercharging for key services. An annual review ensures you’re getting paid fairly.
The most powerful long-term strategy is knowing when it’s time to call in the pros. Outsourcing these headaches to a dedicated RCM partner is the clearest path to scaling your efforts and ensuring every part of your medical practice revenue cycle management is optimized by specialists.
Frequently Asked Questions About Medical RCM
Even with a comprehensive guide, practical questions always pop up when you’re staring down a process as complex as medical RCM. Here are some straight-to-the-point answers to the questions we hear most often from practice managers.
What Is the Most Important Metric in Revenue Cycle Management?
While you need to track several KPIs, your Clean Claim Rate is arguably the most critical one. Think of it as your first-pass success rate—it’s the percentage of claims paid on the very first submission without rework. A high rate, ideally over 90%, tells you that your front-end processes are rock-solid. It’s the ultimate indicator that you’re preventing costly denials and delays before they even start. Nailing this single metric sends a positive ripple effect across your entire revenue cycle.
Can a Small Medical Practice Afford to Outsource RCM?
Yes, and honestly, smaller practices often see the biggest benefits. Outsourcing takes the high, fixed costs of hiring, training, and keeping a specialized billing team and turns them into a predictable, variable expense. Even better, partnering with a nearshore expert gives you access to enterprise-grade technology and deep expertise that would be completely out of reach otherwise. It’s a direct and immediate boost to your bottom line, often paying for itself just by plugging revenue leaks.
How Does a Bilingual Team Improve Patient Collections?
In communities with diverse populations, clear and empathetic communication is everything when it comes to patient collections. When a patient can talk through their bill and payment options in their native language, it instantly cuts through confusion and builds trust.
A bilingual team can turn a collections call—a moment that’s often full of friction—into a positive, helpful conversation. This doesn’t just improve the patient experience; it dramatically increases the odds of getting paid on time.
What Is the Difference Between Medical Billing and RCM?
This is a common point of confusion, but the distinction is crucial. Medical billing is just one piece of the much larger Revenue Cycle Management puzzle.
- Medical Billing: This is the specific, transactional job of submitting claims to insurance companies and chasing down payments.
- Medical Practice Revenue Cycle Management (RCM): This is the entire, end-to-end financial strategy. It starts the moment a patient schedules an appointment and doesn’t end until the final payment is collected—covering everything from denial management to payment posting in between.
A winning RCM strategy looks at the whole financial journey, not just the single transaction of billing.
20px;border-radius:12px;margin-top:24px;text-align:center;”>
🚀 Strengthen Your Revenue Cycle With CallZent
CallZent helps healthcare organizations improve medical practice revenue cycle management with nearshore support for patient communication, back-office workflows, denial follow-up, and billing-related operations.
At CallZent, we specialize in providing the expert support needed to manage every stage of your medical practice revenue cycle management. From accurate patient registration to persistent denial follow-up, our nearshore teams act as a seamless extension of your practice, helping you boost revenue and focus on what truly matters—your patients. Learn more about our custom-fit BPO solutions at https://callzent.com.










